Knee Replacement Surgery
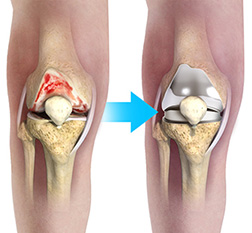
The knee is made up of the femur (thigh bone), the tibia (shin bone), and patella (kneecap). The meniscus, the soft cartilage between the femur and tibia, serves as a cushion and helps absorb shock during motion. In the presence of arthritis, where the cartilage has worn out, the knee can become very painful with symptoms of giving way, stiffness and swelling. In this scenario Knee replacement surgery is a reasonable option. Mr Patel is able to perform computer-aided surgery and is also able to use patient specific instrumentation for a more bespoke surgical procedure.
The goal of total knee replacement surgery is to relieve pain and restore the alignment and function of your knee.
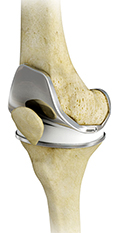
The surgery is performed under spinal or general anaesthesia. Mr Patel will make an incision in the skin over the affected knee to expose the knee joint. Then the damaged portions of the femur bone are cut at appropriate angles using specialised jigs. The femoral component is attached to the end of the femur with or without bone cement. Mr Patel then cuts or shaves the damaged area of the tibia (shinbone) and the cartilage. This removes the deformed part of the bone and any bony growths, as well as creates a smooth surface on which the implants can be attached. Next, the tibial component is secured to the end of the bone with bone cement or screws. Mr Patel will place a plastic piece called an articular surface between the implants to provide a smooth gliding surface for movement. This plastic insert will support the body’s weight and allow the femur to move over the tibia, similar to the original meniscus cartilage. The femur and the tibia with the new components are then put together to form the new knee joint. To make sure the patella (knee cap) glides smoothly over the new artificial knee, its rear surface is also prepared to receive a plastic component. With all the new components in place, the knee joint is tested through its range of motion. The entire joint is then irrigated and cleaned with a sterile solution. The incision is carefully closed, drains are inserted and a sterile dressing is placed over the incision.
Mr Patel performs ‘enhanced recovery’ allowing patients’ to start using their knee earlier and returning home faster. Rehabilitation begins immediately following the surgery. You will be taught specific exercises to strengthen your leg and restore knee movement. Knee immobilisers are used to stabilise the knee. You will be able to walk with crutches or a walker. You will be introduced to a home exercise program to strengthen the thigh and calf muscles.
This helps reduce post-operative complications such as chest infections, urine infections and deep vein thrombosis. Mr Patel does not use a tourniquet, which also helps in post-operative rehabilitation and reduces the risk of thrombosis and post-operative bleeding. After their operation patients’ will work very closely with a specialised physiotherapy team to ensure all their goals are met prior to discharge.
Risks of a total knee replacement include; infection, bleeding, pain stiffness, nerve and vessel damage, thrombosis, fat embolism, fracture, loosening, revision surgery and anaesthetic risks. The risks of these complications are very low and you will not be offered a knee replacement unless the benefits outweigh the risks.